Understanding Your Spine
The intervertebral discs are located between each vertebrae in the spinal column. Of the vertebra, there are 7 cervical (neck), 12 thoracic (mid-back) and 5 lumbar (low back) discs. The discs make up approximately 1/3 of the spinal column. They have three main functions: (1) “Absorb shock” from everyday wear and tear. (2) Allow movement of our spinal column. (3) Separate the vertebrae.
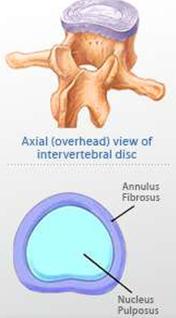
The intervertebral disc is actually a type of cartilaginous joint. Discs consist of an outer layer, annulus fibrosis, and an inner nucleus pulposus, which is a soft, jelly-like, substance. The disc is made up of proteins called collagen and proteoglycans that attract water. Normally, discs compress when pressure is put on them and decompress when the pressure is relieved. These disc do not have a blood supply; therefore, they exchange nutrients by a process called “imbibition”. Imagine a sponge filled with water; when that sponge is compressed, the water is forced out of the sponge. When the compressive force is removed, the water is “sucked” back into the sponge. This is precisely how discs stay healthy and functional. Diseased discs can lead to degenerative disc disease that can then lead to : arthritis, herniated discs, bulging discs, facet syndromes, sciatica and spinal stenosis.
A herniation describes an abnormal condition of an intervertebral disc. Some refer to this condition as a “slipped”, “ruptured”, or “blown” disc. Most of the time it is not known what caused the disc to herniate, but it is thought to occur from repetitive stress due to occupation, poor spinal posture, and/or natural processes of aging and/or trauma.
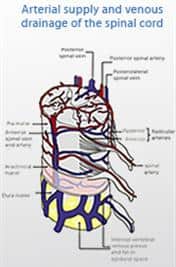
A herniation begins when the inner nucleus pulposus bulges through the annulus fibrosis, causing a bulging or protruding disc. This bulge may push on a spinal nerve. This interferes with the natural blood supply to the nerve roots and sets up a condition known as intraneural edema. Basically, the nerve root microcirculation is compressed and can progress to the point where the nucleus begins to leak out of the disc. At this point the body begins to fight back by launching an autoimmune response to the disc material (nucleus pulposis). The reaction of this defense mechanism causes severe inflammation and progressive deterioration of the nerve root. If the herniation is located in the cervical spine (neck), the symptoms can range from neck pain, with or without arm pain, to numbness and tingling. Muscle weakness can be common as well. If the herniated disc is located in the lumbar spine (low back), the symptoms can range form low back pain, with or without leg pain, to numbness and tingling. Muscle weakness is also common. This type of pain and/or numbness in the legs or arms is referred to as a “radiculopathy”. This happens because the nerves that exit your spinal cord innervate (“attach to”) the skin in your arms and legs. They are responsible for sensation and for movement of the muscles in your arms and legs. They are also responsible for the reflexive movements as well. This is the reason some individuals with there conditions experience extremity (leg/arm) pain / numbness / tingling and/or weakness when they have a herniated or bulging disc. Be aware that, some individuals with herniated discs may report arm or leg pain only, with minimal neck or low back pain.
- Leg Pain / Sciatica
This pain is most commonly experienced at the outside of the thigh, the lower leg and/or foot. Shooting pain that radiates down the leg is a common experience with herniated discs. Patients commonly report an electric shock type of symptoms. - Muscle Weakness
Signals from the brain may be interrupted due to nerve irritation. This can cause muscle weakness, usually of the ankle. Nerve irritation can be tested by examining the reflexes of the knee and ankle. - Parasthesias
This is the medical word for abnormal sensation such as tingling numbness, weakness or “pins and needles”. These symptoms may be the result of a herniated disc and may be experienced in the same regions as painful sensations. - Bowel or Bladder Problems
These symptoms are important because they may be a sign of Cauda Equina syndrome. This condition is possibly caused by a herniated disc. This is a medical emergency! You must see a medical doctor immediately if you have problems urinating, having bowel movements, or if you have numbness around your genitals. All of these symptoms are likely caused by irritation of one the nerves as a result from a herniated disc.


Herniated Disc Diagnosis
Diagnosis of a herniated disc (either neck or low back) can be made from a thorough physical examination including a detailed history, orthopedic and/or neurological evaluation. Some disc patients will present with an antalgic gait (lean away from the side of the disc lesion), extremity pain/numbness/tingling (abnormal sensation) in addition to neck or low back pain. Muscle weakness may be present in the more chronic cases as well as areflexia (“loss of reflex”). X-ray can be helpful in identifying degenerative changes of the vertebra, but MRI’s are the “gold standard” to identify the exact nature of the lesion. When the disc is herniated in the lumbar spine (low back), and it is compressing the spinal nerve roots causing pain and numbness down the buttocks, thigh and leg, it is often referred to as sciatica.
Traditional Treatments
Traditional treatments for herniated discs include physical/chiropractic therapy, epidural injections, surgery, and painkillers such as non-steroid anti-inflammatory medication (NSAIDs).
Please keep in mind that NSNSAIDsave an inherent risk of gastrointestinal (GI) (“stomach” and “intestinal”) disorders such as perforation, ulceration, and hemorrhages. The New England Journal of Medicine reported that it has conservatively estimated that 16,500 NSAID-related deaths occur every year in the United States, and conservative calculations estimate that approximately 107,000 Americans are hospitalized every year due to NSANSAID-related complications. The number of deaths reported in the same study due to AIDS was 16,685. In addition to gastrointestinal disorders, drugs such as VIOXX have been known to cause serious cardiovascular (CV) events such as heart attacks, strokes, and heart failure. There have been similar complaints from other NSAIDs, such as Bextra and Celebrex.
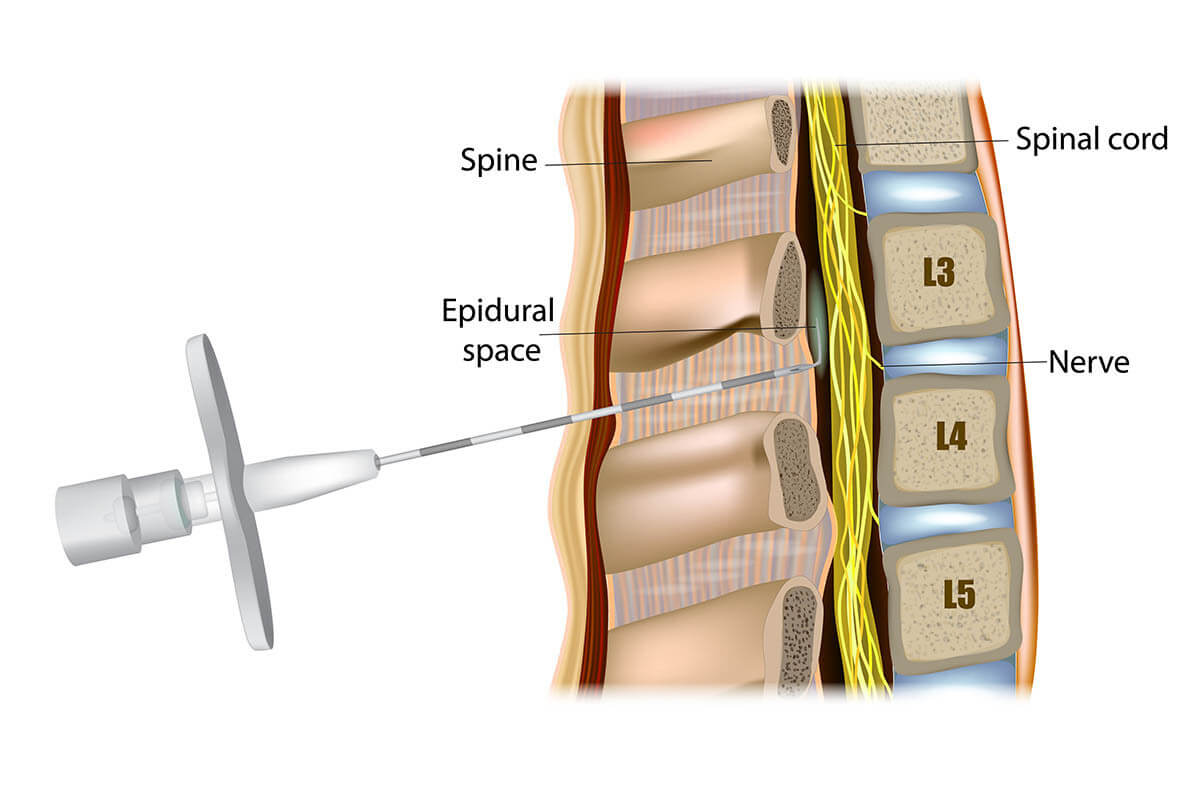
Epidural Injection
Epidural injections (“injection within the epidural space of the spinal cord”) with corticosteroids, lidocaine or opioids have no proven benefit in treating neck or upper back symptoms. In the instances that people find improvement, the effects are often temporary and require repeat injections, and several per year are not uncommon. There is also an increase in risk in contracting a spinal infection that can lead to meningitis. In fact, the results of a randomized, double-blind trial, published in the June 2003 issue of the Annals of Rheumatic Diseases indicated that an epidural steroid injection was not better than an epidural saline (“salt water”) injection (i.e. placebo) for sciatica. These findings are consistent with those of another definitive trial presented at the last American College of Rheumatology meeting.
Given that there have been advances in spinal surgery, the outcomes can still be very unpredictable. In failed back surgery, post-operative pain syndrome is a very disabling and troubling reality of surgical intervention. According to the 2002 Johns Hopkins White Paper on “Low Back Pain and Osteoporosis”* by John P. Kostulk, M.D. and Simeon Margolis, M.D., PhD., surgery “is not the treatment of choice for most people with back pain.” The report goes on to say “fewer than 5% of people with back pain are good candidates for surgery”. “Surgery ought to be used when all other measures have been explored, and only if it appears that there is a strong probability that it will improve the condition.” An article in Spine reviewed the outcomes and complication rates for surgical intervention in degenerative disc disease. Complication rates were as high as 55% and included: hematoma, neurologic adjacent segment degeneration, infection and hardware/instrument-related issues. Another study determined the effects of single-level (2 vertebra) land 2-level (3-4 vertebra) spinal fusion success rates reported 53% with “good” and “fair” results with single-level fusion and no “good” results with 2-level fusions.
Having read about the possible side effects relating to these “traditional” treatments, you might consider the drugless, non-surgical approach that our exclusive DiscHealingSolution® has to offer.
DiscHealingSolution®
DiscHealingSolution® offers a drug-free, non-surgical solution focused on the body’s ability to heal itself. It is designed to:
Relieve pressure on discs and nerves
Restore proper nutrient flow through imbibition
Create negative intradiscal pressure (vacuum effect) to retract disc material
How It Helps:
Reduces or eliminates limb pain and numbness
Decreases nerve inflammation
Promotes long-term healing and mobility
Core Concepts of DiscHealingSolution®:
Spinal decompression
to reduce internal disc pressure
Vacuum effect
to draw disc material inward
Enhanced circulation
to nourish discs and nerves
If you're searching for a safer, holistic alternative to back surgery, DiscHealingSolution® may be right for you.
Sources
- Wolfe et al. Gastrointestinal Toxicity of NSAIDs, NEJM, 1999
- Singh G. NSAID Gastropathy, Am J Med, 1998
- Solomon SD et al. Celecoxib and Cardiovascular Risk, NEJM, 2005
- Kostulk JP. Johns Hopkins White Paper on Low Back Pain, 2002
- Annals of Rheumatic Diseases, 2003 – Epidural study
Conditions We Treat
Each of the following conditions is a result of one core problem—something we identify and explain clearly during our consultation.
Sciatica
The sciatic nerve forms from multiple spinal nerve roots and travels from your lower back down through your legs. When compressed or inflamed, it causes pain, numbness, or tingling.
Herniated Disc
A disc herniation can result from repetitive stress, poor posture, trauma, or aging. It’s often called a “slipped” or “ruptured” disc and can cause serious, lasting pain.
Bulging Disc
Often used as a general term, a “bulging disc” usually refers to a herniated disc. There are two types: broad-based and focal herniations. We help you understand what’s really happening.
Degenerative Disc Disease
As we age, the discs between our vertebrae lose hydration and elasticity. This process can accelerate with certain jobs, injuries, or genetic factors, leading to chronic discomfort.
Spinal Stenosis
Common in adults over 50, this condition involves the narrowing of the spinal canal, which can compress nerves and lead to various symptoms depending on the location and severity.
Numbness & Tingling
These sensations in the arms, hands, legs, or feet often indicate nerve compression from a damaged disc. Early evaluation is key to preventing further damage.
